Watching someone you care about struggle with substance use brings up so many confusing and painful questions. One of the biggest is, “Why can’t they just stop?” It’s a question that can lead to frustration, blame, and misunderstanding. You might wonder if it’s a matter of willpower, a series of bad choices, or something else entirely. The debate over whether addiction is a disease or a choice is more than just a question of words; it shapes how we approach treatment, recovery, and our own feelings of compassion.
If you’re feeling lost in this debate of “is addiction a disease?”, you’re not alone. Understanding the nature of addiction is the first step toward finding a path to healing, both for the person struggling and for those who love them. Let’s take a compassionate look at what the science says and what it means for recovery.
The Disease Model of Addiction
It can be tough to wrap your head around, but leading medical organizations have come to a clear consensus. The disease model of addiction frames substance use disorder as a chronic, relapsing brain disease, not a moral failing. According to experts like the American Society of Addiction Medicine, addiction involves deep-seated changes in brain circuits, genetics, and life experiences. Thinking about it this way helps remove the shame and stigma that can be such a huge barrier to people seeking help.
This doesn’t mean personal choices don’t play a role. They do, much like in other chronic diseases such as heart disease or type 2 diabetes. For those conditions, genetic predisposition, lifestyle choices, and environmental factors all come together. Addiction works the same way. A person doesn’t choose to develop the disease, but they are responsible for managing it through treatment and healthier behaviors. Viewing addiction as a treatable health condition opens the door for real, effective treatment and lasting recovery.
Changes in the Brain
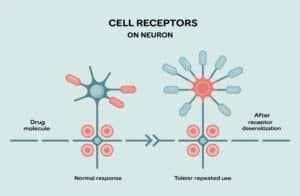
When substances are used repeatedly, they physically change the brain’s structure and chemistry. This is not a metaphor, it’s a neurobiological fact. The most significant changes occur in the brain regions responsible for reward, decision-making, and impulse control. Your brain has a reward system designed to make you feel good when you do things that help you survive, like eating or spending time with loved ones. It releases a chemical called dopamine, which creates feelings of pleasure.
Drugs and alcohol hijack this system, flooding the brain with far more dopamine than natural rewards ever could. Over time, the brain adapts by producing less dopamine on its own and reducing its sensitivity. This is why a person eventually needs the substance just to feel normal and finds little pleasure in everyday activities. These changes create intense cravings and a compulsive drive to use that can feel impossible to resist with willpower alone, often complicating co-occurring mental health and substance use conditions.
Risk Factors
Not everyone who uses substances develops an addiction, and that’s because some people are more vulnerable than others. This isn’t about being “weak,” it’s about having a different set of risk factors that can tip the scales. Understanding these factors helps us see addiction not as a personal failure, but as a health issue that can affect anyone, given the right circumstances.
- Genetics: Family history plays a significant role. Studies suggest that genetics can account for up to half of a person’s risk for developing a substance use disorder.
- Environment: Growing up in a home with substance use, experiencing trauma or chronic stress, and early exposure to drugs or alcohol can all increase a person’s vulnerability.
- Mental Health: Conditions like depression, anxiety, or PTSD often go hand-in-hand with addiction. Many people start using substances as a way to self-medicate the symptoms of an untreated mental health disorder.
These factors don’t guarantee that someone will develop an addiction, but they do create a higher risk. You can learn more about the specific risk factors for addiction to better understand how they contribute to this complex disease.

Is Substance Use a Choice?
This question is at the heart of the matter. The first time a person tries a substance, it is almost always a choice. But for individuals with the risk factors we just discussed, that initial choice can set off a chain reaction that is incredibly difficult to stop. As repeated substance use changes the brain, the ability to choose freely becomes compromised. It’s like a switch gets flipped. What started as a voluntary act slowly transforms into a compulsion.
The brain’s reward system becomes so dependent on the substance that it overrides rational thought. The person isn’t choosing the drug over their family, job, or health; their brain is telling them they need it to survive. This is why shaming or punishing someone often makes things worse. Understanding this shift from choice to compulsion is a critical step toward healing. Our intensive outpatient programs are designed to help you regain control and rebuild your decision-making abilities.
Are People with Addiction Responsible for Their Actions?
This is a sensitive but important question. It’s crucial to separate blame from responsibility. A person is not to blame for having the disease of addiction, just as someone isn’t to blame for having diabetes. However, they are responsible for their actions and for taking steps to manage their health. A person with diabetes must monitor their blood sugar, take their insulin, and manage their diet. Similarly, a person with addiction is responsible for seeking treatment and engaging in their recovery.
Accountability is a cornerstone of recovery, but it must be approached with compassion, not shame. Holding someone responsible for their actions means empowering them to make positive changes and supporting them as they learn to manage their disease. It’s about looking forward to the hard work of recovery, not backward at past mistakes.
Why Do Some People Say Addiction is Not a Disease?
Despite the scientific evidence, some people still argue that addiction is a matter of poor choices or a moral failing. These views often stem from frustration and a misunderstanding of the profound ways substances change the brain. Arguments centered on a “lack of willpower” don’t account for the fact that addiction impairs the very part of the brain responsible for impulse control and sound decision-making.
Societal stigma also plays a huge role in keeping these outdated ideas alive. For centuries, people struggling with substance use have been viewed with judgment rather than compassion. While the debate may continue in some circles, the overwhelming medical and scientific consensus is clear: viewing addiction as a disease provides the most effective and compassionate framework for treatment and recovery.
Frequently Asked Questions
Yes, addiction is considered a chronic disease that affects brain function and behavior. It is classified as a substance use disorder and a mental health condition. Over time, repeated drug use or alcohol use can change brain circuits, making it harder to control cravings and stop using despite harmful consequences.
Drug addiction develops when repeated drug use leads to changes in the brain that reinforce continued use. What may begin as occasional drug misuse can turn into dependence, where a person experiences withdrawal symptoms and feels unable to stop. Over time, addiction can take over a person’s life, affecting relationships, work, and overall well being.
Addiction affects brain circuits, especially those involving dopamine receptors and the prefrontal cortex, which controls decision making and impulse control. Over time, substance use can create intense focus on obtaining and using drugs, making it harder to control cravings. Brain imaging studies show that these changes can impact day to day life and lead to harmful consequences.
Addiction treatment typically involves a combination of therapies and support systems. This can include counseling, behavioral therapy, and structured programs like residential treatment or intensive outpatient programs. A personalized treatment plan helps address both substance use and any underlying mental health conditions, supporting long-term recovery.
Finding Hope and Healing in Recovery
While a significant number of people may develop a substance use disorder, professional treatment greatly improves the chances of lasting recovery. Learning strategies for relapse prevention is a key part of this process, giving you the tools to navigate challenges and stay on track. You don’t have to do this alone; help is here.
Recovery is a process of reclaiming control and rebuilding a life of purpose. It takes courage, but you don’t have to face it alone. The most important step is the first one, reaching out for help.
If you or a loved one is struggling, support is available. Call us today at (484) 517-3005 to speak with someone who understands. We at MPower Wellness of Exton are here to provide the compassionate care you deserve. You can also contact us to begin the conversation.
Sources
- Substance Abuse and Mental Health Services Administration. (July 28, 2025). SAMHSA Releases Annual National Survey on Drug Use and Health. Substance Abuse and Mental Health Services Administration.
- Substance Abuse and Mental Health Services Administration. (December 22, 2025). Co-Occurring Disorders and Other Health Conditions | SAMHSA. Substance Abuse and Mental Health Services Administration.
- Substance Abuse and Mental Health Services Administration. (2025). [PDF] Highlights for the 2024 National Survey on Drug Use and Health. Substance Abuse and Mental Health Services Administration.
- Substance Abuse and Mental Health Services Administration. (October 10, 2023). Key Substance Use and Mental Health Indicators in the United States. Substance Abuse and Mental Health Services Administration.
- American Society of Addiction Medicine. (September 15, 2019). What is the Definition of Addiction – ASAM. American Society of Addiction Medicine.
- National Institute on Drug Abuse. (July 6, 2020). Drugs, Brains, and Behavior: The Science of Addiction. National Institute on Drug Abuse.
- Substance Abuse and Mental Health Services Administration. (June 9, 2023). National Helpline for Mental Health, Drug, Alcohol Issues – SAMHSA. Substance Abuse and Mental Health Services Administration.
- National Center for Biotechnology Information. (January 1, 2006). Chapter 8. Intensive Outpatient Treatment Approaches – NCBI – NIH. National Center for Biotechnology Information.
- Substance Abuse and Mental Health Services Administration. [PDF] Low Barrier Models of Care for Substance Use Disorders. Substance Abuse and Mental Health Services Administration.
- Hser, Y. I., Evans, E., Grella, C., Ling, W., & Anglin, D. (2015). How Many Recovery Attempts Does it Take to Successfully Resolve … . National Library of Medicine.
- Minozzi, S., Saulle, R., De Crescenzo, S., & Amato, L. (2017). Summary of Evidence – Inpatient and Outpatient Treatment … – NCBI. National Center for Biotechnology Information.