It might surprise you to learn that genetic factors can influence 40 to 70 percent of a person’s addiction risk, turning the common belief that it’s just about willpower on its head. Addiction isn’t a moral failing, it’s a chronic condition of the brain, like diabetes or asthma, and it has a way of creeping in over time, layer by layer. By shedding light on the stages of addiction, you’ll start to see that this journey isn’t hopeless; knowledge is the first, most powerful step toward finding help that truly understands and supports you.
The Stages of Substance Abuse and Addiction
When you’re in the middle of it, addiction can feel like a sudden crisis that appeared out of nowhere. But in reality, it’s almost always a gradual process, a slow slide with distinct phases. Think of it less like falling off a cliff and more like walking down a long, sloping path that gets steeper and harder to climb back up over time. Understanding the stages of addiction helps you see where you or a loved one might be on that path.
It’s important to remember that not everyone who tries a substance will travel through every stage. Many people stop at the early phases. But recognizing how the addiction cycle works is the key to catching it early, before it takes hold completely. We’ll walk through each of these stages, from the very first use to the point where it becomes a substance use disorder, so you can see the full picture.
Stage 1: Initiation
This is the very beginning, the first time a person tries a substance. For many, this initial use happens during adolescence. It might be driven by simple curiosity, a desire to fit in with friends, or peer pressure. For others, it’s a way to cope with something difficult, like stress, anxiety, or physical pain. The National Institute on Drug Abuse (NIDA) has found that most people who develop an addiction tried their substance of choice before they turned 18. This first step doesn’t guarantee a future problem, but it’s the entry point where risk factors, such as genetics and a person’s home environment, start to play a crucial role.
Stage 2: Experimentation
After the first try, a person might move into a stage of experimentation. Here, the substance use is still irregular and often happens in social settings, like at parties or on weekends with friends. There isn’t a predictable pattern yet, and the person likely feels they are in complete control. Because there are few, if any, significant negative consequences at this point, it’s easy to believe that casual use is harmless. The real danger in this stage is the normalization of the behavior and the tendency to underestimate just how powerful and addictive some substances can be.
Stage 3: Regular Use
Experimentation can slowly shift into regular use, which is defined by a predictable pattern. Maybe it’s drinking every evening after a stressful day at work, or using a substance every weekend without fail. The substance is no longer just for special occasions; it has become integrated into the person’s routine. You might notice subtle shifts happening. Their social circle may change to include more people who use substances, leading to a degree of social isolation from old friends. This is also when family members or close friends often start to voice their concerns as they notice the habit forming and the person changing.
Stage 4: Risky Use
At this stage, the person continues to use the substance even when it’s causing clear, negative consequences. These consequences can show up in any area of life, from slipping grades at school to poor performance at work to strained relationships to legal trouble. High-risk behavior becomes more common, such as driving under the influence or prioritizing getting and using the substance over major responsibilities. The use is no longer just a habit; it’s becoming a serious problem that impacts their safety and the well-being of others. If this sounds familiar to you or someone you care about, it’s a sign that it’s time to talk to someone.
Stage 5: Dependence
Dependence is when the body has adapted to the presence of the substance and needs it to feel “normal.” This can be both physical and psychological. Physical dependence means that if the person stops, they will experience withdrawal symptoms, which can range from uncomfortable to life-threatening. Common symptoms include anxiety, shakiness, nausea, and irritability. At the same time, their tolerance has likely increased, meaning they need more of the substance to get the same effect. It’s important to understand that dependence isn’t the same as addiction, but it is a powerful force that often fuels it, making it incredibly difficult to stop.
Stage 6: Addiction
The final stage is addiction, which is clinically known as a substance use disorder (SUD). This is defined by a loss of control and compulsive use, even in the face of severe consequences to one’s health, finances, and relationships. According to the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), a substance use disorder is diagnosed based on 11 criteria. At this point, the substance has become the central focus of the person’s life. They may give up hobbies they once loved, withdraw from family, and ignore all other responsibilities. Their behavior is no longer a choice in the traditional sense; it’s driven by a powerful compulsion that has hijacked their brain.
The Primary Brain Regions Involved in Substance Use Disorders
When we say addiction is a brain disease, it’s not a metaphor. Chronic substance use physically changes the brain’s structure and how it functions. It essentially hijacks the systems meant to help us survive, such as those for reward, motivation, and memory. Instead of driving us toward healthy behaviors like eating and connecting with others, it wires the brain to prioritize the substance above all else. To understand how this happens, let’s look at the three key areas of the brain that are most affected.
The Basal Ganglia
Often called the brain’s reward circuit, the basal ganglia is responsible for motivation, pleasure, and turning our actions into habits. When you do something enjoyable and healthy, like eating a good meal or spending time with people you love, this area releases a small amount of dopamine, which makes you feel good and helps your brain learn to repeat the behavior.
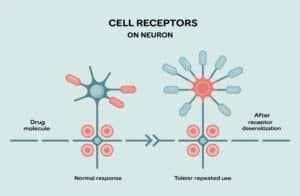
Addictive substances flood this system with a massive, unnatural surge of dopamine release, creating an intense feeling of euphoria. With repeated use, the brain adapts by becoming less sensitive to both the substance and everyday pleasures. This is why substance use can become a compulsive habit, driven less by the pursuit of pleasure and more by a deeply ingrained, almost automatic routine.
The Extended Amygdala
Think of the extended amygdala as the brain’s “alarm” system. It’s responsible for our response to stress, fear, and anxiety. In a healthy brain, it helps us avoid danger. But as the pleasurable effects of a substance decrease with repeated use, this stress system becomes overactive during withdrawal. When a person isn’t using the substance, they can experience negative feelings like irritability, unease, and anxiety. This creates a powerful motivation to use the substance again, not to feel good, but simply to get relief from these uncomfortable feelings. This is a process called negative reinforcement, and it’s a key driver in the addiction cycle.
The Prefrontal Cortex
Located at the very front of the brain, the prefrontal cortex is our “stop” system. It’s responsible for executive functions such as decision-making, problem-solving, and impulse control. It’s the part of the brain that allows you to think through the consequences of your actions and make rational choices.
Addiction weakens this region, making it much harder to resist the intense cravings and impulses coming from the basal ganglia and extended amygdala. This impairment explains one of the most confusing aspects of addiction: why a person might continue to use a substance even when they know it’s causing devastating harm to themselves and others. Their ability to say “stop” is compromised.
What Are the Signs of Addiction?
Recognizing the signs of addiction isn’t always straightforward, as they can be subtle at first and grow more obvious over time. These symptoms of addiction fall into a few key categories, and seeing a pattern of them is a strong indicator that it’s time to seek help. According to the DSM-5, the clinical manual used to diagnose substance use disorders, the number of symptoms a person shows helps determine whether the condition is mild, moderate, or severe.
Here are some of the most common signs to watch for:
- Behavioral Signs:
- Increasing secrecy, lying about substance use, or hiding it from others.
- Withdrawing from friends and family or suddenly changing social circles.
- Losing interest in hobbies and activities that were once important.
- Neglecting responsibilities at work, school, or home.
- Having financial troubles, like borrowing or stealing money to pay for substances.
- Physical Signs:
- Significant changes in appearance, such as neglect of personal hygiene or sudden weight loss or gain.
- Bloodshot eyes, pupils that are larger or smaller than usual.
- Changes in sleep patterns, like insomnia or sleeping at odd hours.
- Experiencing withdrawal symptoms (like nausea, sweating, or tremors) when not using the substance.
- Psychological Signs:
- Unexplained mood swings, increased irritability, or outbursts of anger.
- Appearing anxious, fearful, or paranoid for no clear reason.
- An inability to stop using the substance, even when wanting to.
- Continuing to use despite knowing it’s causing or worsening physical or mental health problems.
Frequently Asked Questions
The five stages of change, part of the Transtheoretical Model, outline a person’s readiness to address their substance use. They help show that recovery is a process, not a single event.
The stages are:
1. Precontemplation: Not yet recognizing a problem.
2. Contemplation: Acknowledging the problem but not ready to change.
3. Preparation: Getting ready to take action soon.
4. Action: Actively changing behaviors and habits.
5. Maintenance: Working to sustain change and prevent relapse.
Individuals move through these stages at their own pace, and understanding them helps tailor treatment and support effectively.
There is no specific timeline for the stages of recovery, as the journey is unique for every person. The process is not linear, and it’s common for individuals to move back and forth between stages before achieving long-term success.
Some people may remain in contemplation for years, while others might move to action quickly after a significant event. The final stage, maintenance, is a lifelong commitment. Focusing on steady progress is more important than trying to meet a deadline, as lasting recovery takes time and patience.
It’s important to remember that relapse is not a failure. For many people with substance use disorders, it can be a part of the long-term recovery process. The most important step is to reach out for support immediately—call your therapist, sponsor, or a trusted loved one. Don’t let feelings of shame or guilt keep you isolated.
A relapse is an opportunity to re-evaluate your treatment plan and identify triggers, such as stress or anxiety, that need to be managed differently. It’s a sign to strengthen your coping skills, not to give up on your progress.
Seeking Help to the Path to Recovery
For some, the first step may be detoxification to safely manage withdrawal symptoms before they can begin the deeper therapeutic work. Afterward, outpatient programs offer a way to get structured, intensive support while still managing daily responsibilities like work or family. At MPower Wellness, we offer different levels of care, including partial hospitalization (PHP), intensive outpatient (IOP), and standard outpatient treatment programs.
A cornerstone of effective treatment involves therapies that address the root causes of addiction. Evidence-based approaches like cognitive behavioral therapy (CBT) and dialectical behavior therapy (DBT) are incredibly effective. CBT helps you identify and change the negative thought patterns and behaviors that fuel substance use, while DBT focuses on teaching skills for emotional regulation and distress tolerance. Since substance use often goes hand-in-hand with mental health conditions like anxiety or depression, our dual diagnosis programs are designed to treat both issues at the same time, which is essential for lasting recovery.
If you’re ready to learn more, the team at MPower Wellness of Exton is here to help. Call us at (484) 517-3005 for a confidential conversation about how our programs can support you, or contact us online to start the process. Taking that step is a sign of strength.
Sources
- National Center for Biotechnology Information. (November 3, 2016). THE NEUROBIOLOGY OF SUBSTANCE USE, MISUSE, AND … – NCBI. United States National Library of Medicine.
- Substance Abuse and Mental Health Services Administration. Client’s Handbook: Matrix Intensive Outpatient Treatment for People …. Substance Abuse and Mental Health Services Administration.
- Substance Abuse and Mental Health Services Administration. Roadmap for Recovery – SAMHSA Library. Substance Abuse and Mental Health Services Administration.
- National Institute on Drug Abuse. (July 6, 2020). Drugs, Brains, and Behavior: The Science of Addiction. National Institute on Drug Abuse.
- National Center for Biotechnology Information. (January 1, 2006). Chapter 3. Intensive Outpatient Treatment and the Continuum of Care. United States National Library of Medicine.
- Centers for Disease Control and Prevention. (May 27, 2021). DSM-5 Criteria and Severity Scale – CDC. Centers for Disease Control and Prevention.
- American Society of Addiction Medicine. DSM-5 Criteria for Diagnosis of Opioid Use Disorder – ASAM. American Society of Addiction Medicine.
- National Center for Biotechnology Information. Cognitive-Behavioral Therapy for Substance Use Disorders – PMC. United States National Library of Medicine.
- National Center for Biotechnology Information. (July 21, 2023). Addiction Relapse Prevention – StatPearls – NCBI Bookshelf – NIH. United States National Library of Medicine.
- Substance Abuse and Mental Health Services Administration. Recovery from Substance Use and Mental Health Problems Among …. Substance Abuse and Mental Health Services Administration.
- Department of Veterans Affairs. (July 26, 2018). Reducing Relapse Risk – Whole Health Library – VA.gov. Department of Veterans Affairs.
- National Association of Addiction Treatment Providers. Addiction Treatment Methods | Evidence-Based Practices. National Association of Addiction Treatment Providers.
- National Institute on Alcohol Abuse and Alcoholism. (May 8, 2025). Neuroscience: The Brain in Addiction and Recovery. National Institute on Alcohol Abuse and Alcoholism.
- Icahn School of Medicine at Mount Sinai. (August 18, 2022). Brain Reward Pathways – Neuroscience Labs. Icahn School of Medicine at Mount Sinai.
- Texas State University. (January 25, 2024). 1.5 Neurobiology of Substance Use Disorders. Texas State University.